4 ways to improve your blood collection technique
Even today, venipuncture is rarely covered in undergraduate courses. However, this is one of the areas where medical staff are most critically evaluated by patients. It is therefore important to use the best and most reliable technique for taking blood samples in all situations.
Besides needlestick injuries, which are mostly preventable, but pose a significant risk to blood collection staff, another common issue is haemolysis. If a blood sample is collected poorly, the results derived from it may be inaccurate or the blood sample may require recollection, which means extra work and inconvenience for both the clinician and the patient. The three major issues resulting from errors in collection are haemolysis, contamination, and inaccurate labelling.1,2 Factors that increase the risk of haemolysis include the use of needles with incorrect gauge, drawing blood specimens from an intravenous or central line, or underfilled tubes.1
Based on these factors, here are four ways to improve your blood collection technique:
1. Know the standards and request training when needed!
As Sharon Scott, a Greiner Bio-One Product & Application Specialist says, “know and follow the standards for blood collection.” The Clinical and Laboratory Standards Institute (CLSI) sets these standards for venous blood collection that are updated regularly.3
Sharon points out that the manufacturer’s instructions for use should always be followed when using blood collection devices, especially when activating the safety mechanism. Also be aware that proper training is required before using new products. In addition, a helpful tip if you fail to collect a specimen is to accompany the person next attempting the collection to learn from them.
2. Consider problematic vein conditions!
There are unfavourable factors which can negatively impact a blood collection. Stress can lead to vasoconstriction in anxious patients. It is therefore important to create a pleasant atmosphere. Even if the room temperature is too low, this can have a negative effect on venipuncture because veins contract when it's cold. Additional factors could be thin veins, veins that have been punctured multiple times before, rolling veins or volume deficiency.
In particular, elderly or dehydrated patients tend to have difficult vein conditions and slow blood flow. If the needle is already in the vein and there is not sufficient venous blood flow, the vacuum of the tube may cause a collapsed vein. As a result, the needle could adhere to the inner vein wall which may result in the blood flow stopping. As a side effect, the tip of the needle could pierce through the vein causing a haematoma.
Greiner Bio-One Product & Application Specialist, Agnieszka Molas-Kilianek, says, “when confronted with a problematic vein, ask the individual if there has been an area that has worked in the past. This one question could save everyone time and energy throughout this process.” Another aspect that can be considered in this context is the amount of blood that is collected, because in some cases it is no longer necessary to collect large amounts of blood. This approach, known as patient blood management, aims to draw only as much blood as is needed and can be particularly beneficial for patients in preventing iatrogenic anaemia.
3. Choose the right product combinations!
The selection of the right products and product combinations can also influence the success of the blood collection. The use of closed systems is generally the preferred option as they are safer than open systems.4
The needle diameter is indicated in gauge (G), which historically meant “measuring rod”. The higher the G number, the thinner the outer diameter of the blood collection needle. This, along with the standardized colour coding, helps to quickly identify the correct needle depending on the vein conditions.5
If the needle is too large for the vein for which it is intended, it may tear the vein and cause bleeding (haematoma); if the needle is too small, it could damage the blood cells during sampling, and laboratory tests that require whole blood cells, or haemoglobin and free plasma, will be invalid.1
The choice of tube size can also affect the success of the blood collection. For example, choosing a high-volume tube for a difficult vein condition can lead to underfilling or to the collapsing of veins. If the tube is not filled to the marked volume, the ratio of additive to blood will be too high, possibly resulting in inaccurate laboratory results.
4. Hand positioning and needle insertion!
If necessary, ask the patient to form a fist so that the veins become more prominent. Patients should not be instructed to vigorously open and close their hand (pumping) as this can cause significant elevations in potassium concentration, risking complications and patient mismanagement.3
Anchor the vein by holding the patient's arm and placing a thumb below the venipuncture site to pull the skin taut in direction of the patient’s wrist.4 This enables accurate penetration of the skin and prevents the vein from “rolling”.
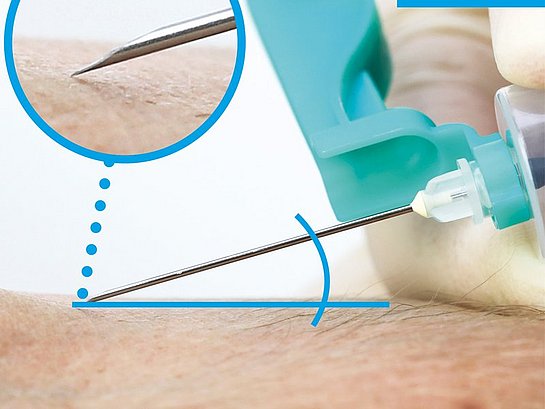
Insert the needle at an angle of ≤ 30 degrees. The needle tip should be facing upwards. In a successful puncture, a decrease in resistance is felt when penetrating the vein wall. The insertion depth can vary depending on the patient and the selected vein.
Hold the tube holder with the thumb and forefinger, using the ridges on the holder for a secure grip. With your free fingers, you can stabilize your hand on the patient’s arm. This allows the tube holder and cannula to be easily inserted and accurately adjusted, preventing further movement of the cannula in the vein, which can cause pain and injury.
While inserting the tube into the holder, the forefinger and middle finger of the other hand are positioned behind the flanges of the tube holder, while the tube is pushed in with the thumb. The rear end of the cannula pierces the stopper in the cap and the blood flows into the tube. This hand position prevents any cannula movement while inserting and pulling out the blood collection tube and avoids the tube sliding off the needle, which could result in underfilling.
If blood is only flowing into the tube hesitantly or not at all, there may be various reasons for this. Minimal re-positioning of the cannula, leaving the blood collection tube attached, can be sufficient to activate the blood flow.
When removing the needle, do not apply pressure to the puncture site until the needle has been completely removed. Otherwise, the needle tip may cut the posterior vein wall, possibly causing pain and a haematoma.
To reduce the risk of needlestick injuries after taking blood, dispose of materials in appropriate sharps disposal containers.
1 WHO guidelines on drawing blood: best practices in phlebotomy, https://www.who.int/publications/i/item/9789241599221
2 International Safety Center, EPINet Report 2021, https://internationalsafetycenter.org/exposure-reports/
3 CLSI. Collection of Diagnostic Venous Blood Specimens, 7th ed. CLSI standard GP41. Wayne, PA: Clinal and Laboratory Standards Institute; 2017.
4 WHO Best Practices for Injections and Related Procedures Toolkit. Geneva: World Health Organization; 2010 https://www.ncbi.nlm.nih.gov/books/NBK138496/
5 Needles – more than just a piece of metal, Greiner Bio-One. https://www.gbo.com/fileadmin/media/GBO-International/02_Downloads_Preanalytics/SALES_Application_Notes/PIENN01_Needles_R00.pdf